How is one of the world’s most innovative hospitals tackling health care’s biggest problem?
Research at Shirley Ryan AbilityLab found a brief emotional intelligence intervention increased doctors’ capacity to avoid burnout.
Physician burnout has been linked to increased medical errors, negative clinical outcomes for patients, and rising healthcare costs. Burnout costs the healthcare system $4.6 billion a year in the US alone. Despite decades of efforts to counteract this issue, physician burnout persists as a pressing problem. In a 2015 study of nearly 7,000 doctors, 54% reported symptoms of burnout – a rate nearly double that of the general population.
Leaders at Shirley Ryan AbilityLab in Chicago – the nation’s top physical medicine and rehabilitation hospital – decided to tackle this problem head on. Inspired by a growing body of research that links emotional intelligence training to increased performance and greater resiliency, the hospital introduced an emotional intelligence training program for first-year medical residents – with promising results.
Shirley Ryan AbilityLab, formerly known as the Rehabilitation Institute of Chicago, is the top-ranked rehabilitation hospital and one of the leading innovators in healthcare. In 2017, the organization opened a $550 million, 1.2-million-square-foot facility, becoming the first-ever “translational” research hospital in which clinicians, scientists, innovators and technologists work together in the same space, surrounding patients, discovering new approaches and applying (or “translating”) research in real time. The goal: better, faster recoveries.
The Chief Medical Officer at Shirley Ryan AbilityLab, Dr. James Sliwa, stresses that the state of the art facilities can only be used to their full potential when the doctors and nurses who fill the building are flourishing and motivated: “The physical space is a manifestation of the people who work in it, and how they work together,” says Dr. Sliwa. “And research shows that emotional intelligence is a critical factor in people’s ability to regulate themselves and work effectively with others.”
After years of practicing the skills of emotional intelligence himself, Dr. Sliwa encountered research on EQ decreasing rates of burnout, and a strategy became clear: Get ahead of the problem. Be proactive in equipping physicians early on with the emotional skills they need to be resilient.
As a result, Dr. Sliwa and team formally introduced EQ training for first-year residents. Working in partnership with Kelli Schulte of EQuip Studios (a leading provider of emotional intelligence training, assessment, and coaching), they designed a measurable pilot project. The goal was a customized, high impact program for the resident MDs, leveraging the SEI (Six Seconds Emotional Intelligence Assessment) to measure the results.
Because of the intense demands of the resident physicians’ schedules, the entire EQ training consisted of a 30-minute introduction to EQ and three 45-minute workshops. In the sessions, Schulte presented the residents with common challenges that arise in healthcare settings (which she gleaned from Dr. Sliwa’s decades of work in the field). Participants discussed how they would typically handle each situation and then collaborated to apply emotional intelligence for a more effective resolution.
In healthcare’s data-driven context, Dr. Sliwa and Ms. Schulte recognized the importance of measuring the program’s impact. The participants took the SEI to kick off the program and again at the end. The results were powerful both in terms of overall emotional intelligence, and the impact on “stretch zone,” a metric in the SEI Group Development Report that is linked to reduced burnout.
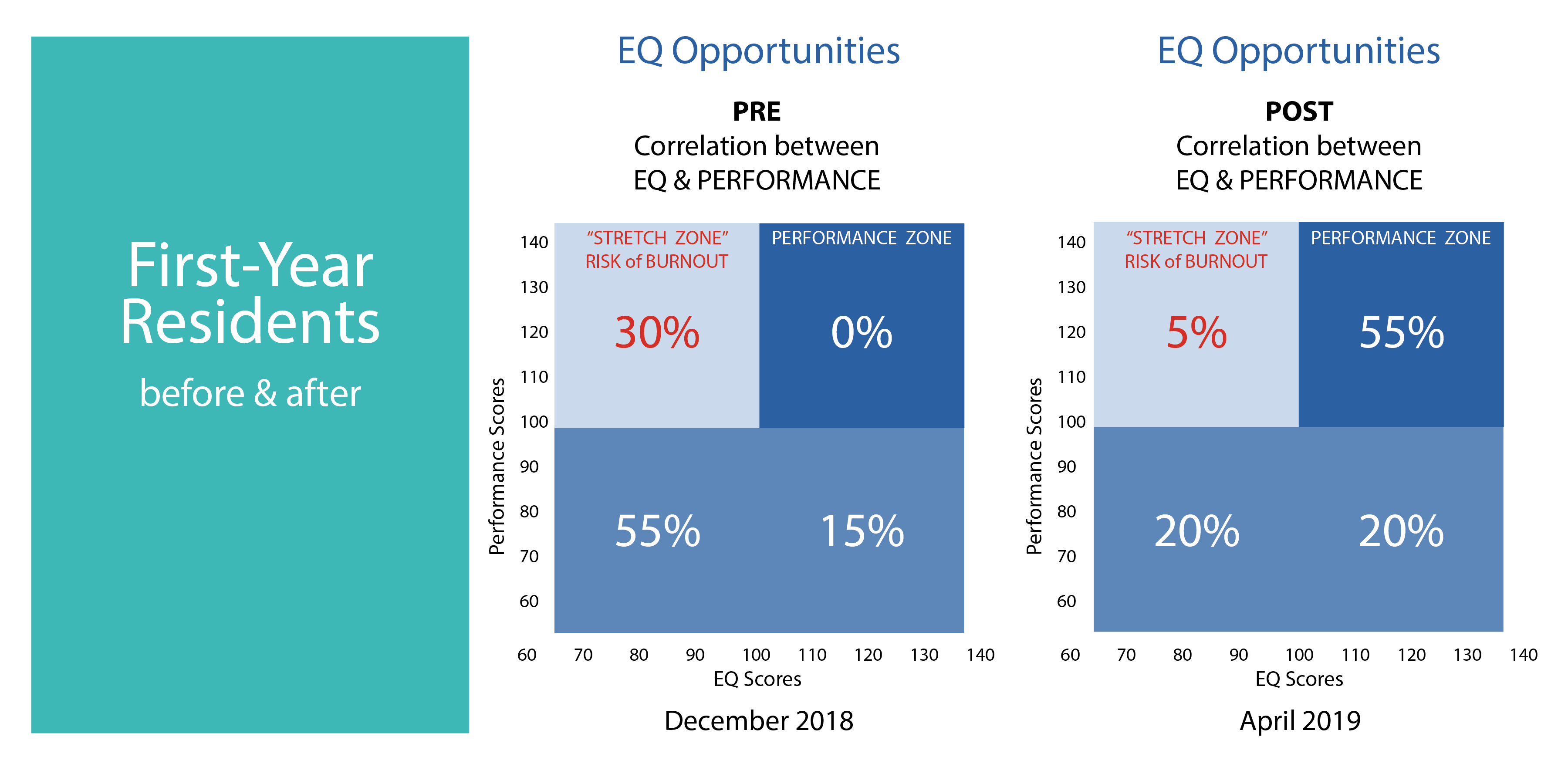
In this summary of pre-post assessments, the 30% in the top-left box are in the “stretch zone” at risk of burnout. This drops to 5% in the post-test. Meanwhile, the number in the peak performance zone (top-right) increased from 0% to 55%, suggesting a massive increase in capability.

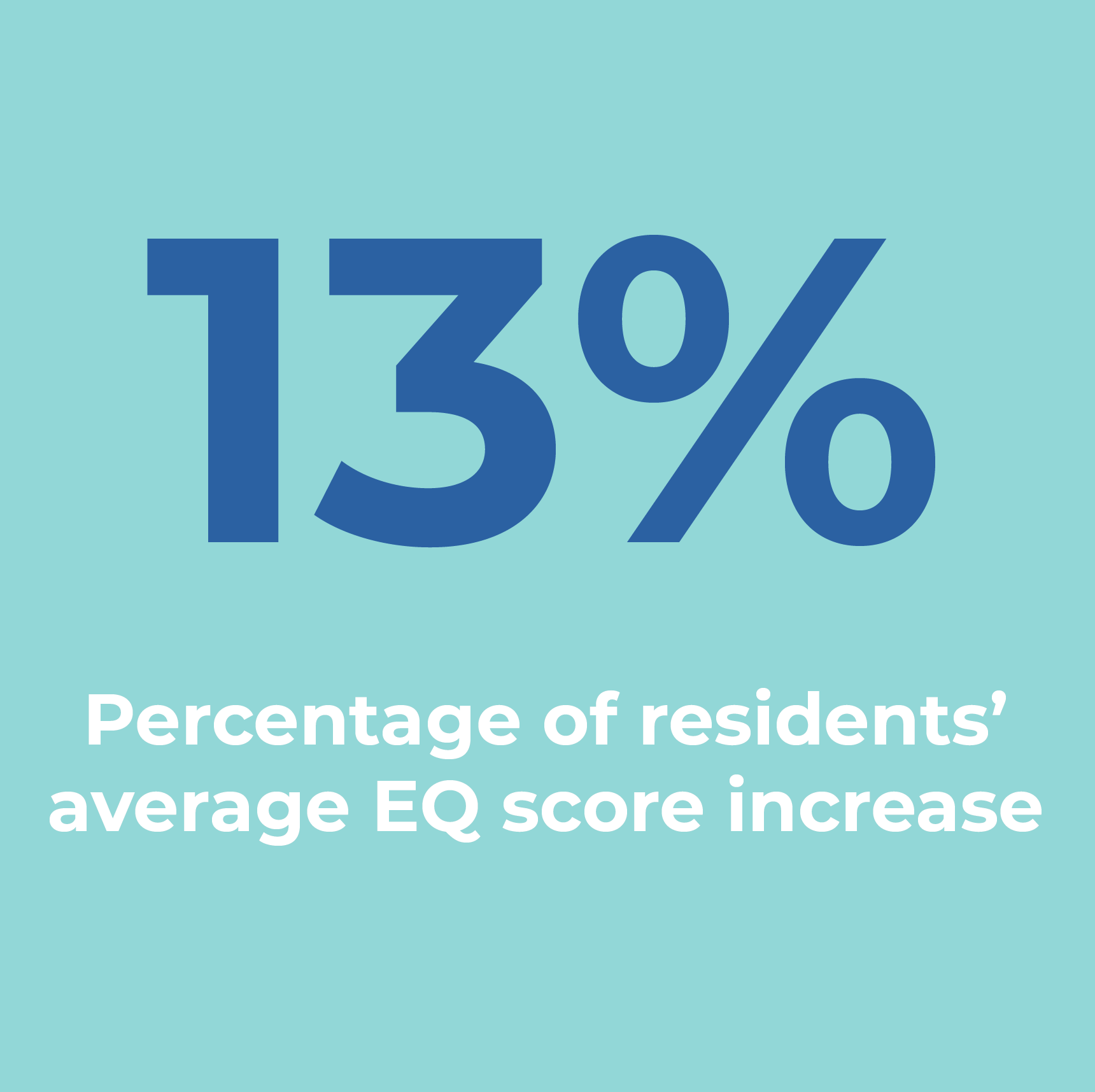
If 13% seems like a modest improvement, consider this: Recent research from Liberty University in Virginia found that its medical students’ emotional intelligence declined during their time in medical school, likely due to the high levels of stress. Considering the growing body of evidence linking doctors’ EQ to both physician and patient success, Dr. Sliwa feels passionately that EQ training must not be overlooked by medical schools: “Our job is to help the residents develop the skills they need to be effective physicians. If you know what emotional intelligence is, you know that it is a crucial element of physician success. These results are promising and we’re looking forward to expanding the program.”
The ROI for EQ is high. “For me,” Dr. Sliwa says, “the big takeaway is that these are measurable, learnable skills, and you can see improvement with even a modest investment of time and energy.”
EQ is learnable. As numerous other case studies have shown, the measurable skills of EQ can be increased. This pilot demonstrates that, in the right conditions, a small effort in EQ makes a massive difference.
People matter. One of the key factors that made this case successful is that Dr. Sliwa and the attending physicians have committed to grow and use their own EQ skills. In the study, 100% of the attending physicians are in that top-right high performance zone shown above.
Latest posts by Michael Miller (see all)
