 Unlocking the Potential to Transformational Change
Unlocking the Potential to Transformational Change
It’s rare to pick up an article on the rapid pace of change in health care today without encountering the word “collaboration.” As healthcare reform unfolds and incentives for reimbursement shift from fee-for-service (do-more-get-more) to one that reimburses for keeping patients healthy (value-based payments), the need to collaborate across departmental, organizational, sector, and community boundaries has emerged in healthcare as never before.
Collaboration involves working across professional boundaries, engaging in joint decision making and sharing ownership of decisions. Here are just a few examples of the shift from competition (or at best coordination) to collaboration across boundaries in healthcare:
 Payers and providers who for decades related primarily through negotiation and competition are recognizing collaboration is an effective route to improving care delivery.[1] At the forefront are hospital networks with health insurance companies and health insurers who are running hospitals to deliver higher quality, value-based care.[2]
Payers and providers who for decades related primarily through negotiation and competition are recognizing collaboration is an effective route to improving care delivery.[1] At the forefront are hospital networks with health insurance companies and health insurers who are running hospitals to deliver higher quality, value-based care.[2]- Rural and large urban hospitals are partnering to consolidate and deliver care.
- The Institute of Medicine recommended that nurses, physicians and other health professionals be full partners in working together to redesign healthcare.[3]
- Public health departments and hospitals are seeking ways to assess community needs and collaboratively develop community health improvement plans.
At the same time, it’s an uphill process. Until recently, collaboration across the spectrum of healthcare has not been highly valued, so few healthcare leaders “grew up” in a collaborative context. “Collaboration needs a different kind of leadership; it needs leaders who can safeguard the process, facilitate interaction and patiently deal with high levels of frustration.”[4]
In other words, since feelings are the drivers or barriers to collaboration, this way of engaging requires emotional intelligence (EQ). As the precursor of collaboration, emotional intelligence is the ability to blend thinking, feeling and acting for optimal decisions. This requires tuning into emotional data, responding intentionally, and using the opportunity to move forward meaningfully.[5]
Certainly, collaboration includes technical and intellectual skills – yet neuroscience shows that collaborating with people is governed by emotion. That’s why working together can be delightfully invigorating or profoundly threatening.
Competing Neural Pathways
Emotional intelligence may be key to collaboration because of two parallel neural pathways that are triggered when two parties sit down to work together (or not).
First let’s look at the bright side. When collaboration goes well, research demonstrates that oxytocin is released. This feel-good-because-you’re-connecting neuro-hormone is released when our thoughts, feelings and actions blend with others. This is the same chemical that is released when a new mother looks into the face of her child, when we pet the dog or cat – or when the team is flowing in synch, like a glorious ballet.
On the other hand, as David Rock points out in Your Brain at Work, when we perceive someone as a competitor or adversary, empathy and oxytocin plummet along with our willingness to explore the validity of other’s ideas, or even hear their ideas.[6] When we evaluate the other person as a threat, a primal stress response is triggered. We put up walls and sharpen our axes.
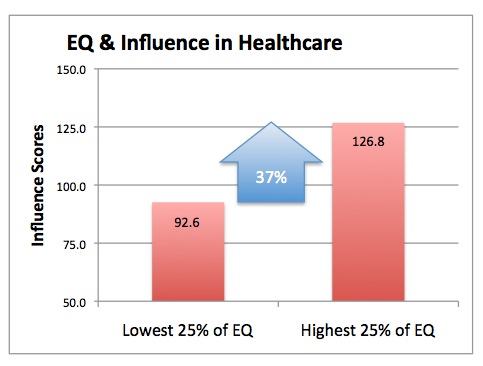
Influence is a key component of collaboration. Research with the Six Seconds Emotional Intelligence Assessment (SEI) on 321 healthcare professionals shows a very strong link between EQ and influence. Those with higher EQ scores also had a 37% advantage on influence.[8]
So, imagine a provider and third party payer are coming together to work on creative solutions for keeping an entire population of patients healthy. For decades their relationship has been characterized by competing commitments and acrimonious negotiations. They’ve been told they have to collaborate – but when they sit down across the table from one another, loaded with decades of defensiveness, are we going to see a ballet or a battle?
The Foundation of Collaboration
It’s easy to say, “we need collaboration,” but if we don’t attend to the underlying emotional requirements, it’s unlikely at best. One key step is building connection. The parties need to FEEL that they have a shared purpose – that they’re on the same team. This is easy to say, but given our history in healthcare, it’s difficult to achieve. Here are three tips when working to shift toward the new frontier of collaboration:
1. Build in time for personal connection. When we meet across the table wearing our roles, we carry our history and thus may automatically scan for threats. When we first create connection through getting to know the person we find that all these people are actually human beings. Through building a personal relationship, a new door opens.
This time is not just “nice to have experienced,” nor is it “wasting time before we get to the real work.” It’s essential ground-breaking – without which, the foundations will be unstable.
2. Choose your emotions. Consider how you want to feel, and how you want others to feel, at the end of each meeting. Pay attention to your emotions and the emotions of others. Noticing and silently naming your emotions can be a powerful way to stay present and move from defensiveness to openness.
3. Engage optimism. An optimistic perspective increases hope, broadens possibilities and supports innovative thinking. Focusing on solutions and desired outcomes, even in the face of significant challenges, helps you see beyond the present to shape the future.
In a nutshell, collaboration has emerged as a critical “doorway” to positive outcomes in healthcare. If we want to achieve the triple aims of reform: 1) enhancing value; 2) improving the health of populations; and 3) reducing costs – collaboration is no longer optional.
While the doorway is now clearly visible, many in healthcare are struggling to get across the threshold to collaborate in new and innovative ways. Since emotional intelligence is a vital key to collaboration and these skills are learnable[7], if we want more collaboration in healthcare, it may be time for a concerted effort to cultivate and integrate these skills.
How are you contributing to positive change in health care through collaboration?
What makes your collaborations successful?
This article was a collaboration between Colette Herrick and Joshua Freedman.
References:
1 Javanmardian, M. Saxena, S.B. “Allies in Values-Based Care.” Trustee: 66:(5) May 2013, 13-16.
2 Nixon, A. A Note for Health Insurers Everywhere: Keep a Close Eye on Pittsburgh, Med City News: Today’s Headlines, www.medcitynews.com, July 29, 2013.
3 Institute of Medicine: Future of Nursing: Leading Change, Advancing Health, (2011), National Academies Press
4 Chrislip, David (2002). The Collaborative Leadership Fieldbook – A guide for citizens and civic leaders. Josey Bass.
5 Freedman, J. (2009) At the Heart of Leadership. Six-Seconds
6 Rock, David. (2006) Your Brain at Work. Harper-Collins
7 Fariselli, Freedman, Ghini (2006). White Paper: Increasing Emotional Intelligence (www.6seconds.org/tools/sei/research)
8 This sample consists of 321 healthcare professionals and senior managers from around the globe, from the SEI norm base in 2011-2012. SEI is a normed, validated assessment of emotional intelligence (www.6seconds.org/sei) Freedman, Jensen, Ghini (2005), The Six Seconds Emotional Intelligence Assessment.
- Leading Kindness: When College Students Practice EQ in Service of Others, Their Own Emotional Intelligence Increases - April 9, 2026
- Emotional Intelligence in Healthcare: A Quick Check-In Guide to Improve Patient Care and Reduce Burnout - November 18, 2025
- Plutchik’s Wheel of Emotions: Feelings Wheel - February 6, 2025






